At a glance
- Lead a learning culture that builds staff confidence, competence, and continuous improvement.
- Ensure mandatory training, competencies, and educational governance are consistently met.
- Provide high-quality learning environments for students through strong supervision and support.
- Collaborate with education teams to align development with service needs and national standards.
Investing in your own professional development
To lead others effectively managers must actively invest in their own professional development. A learning culture begins with the leader: your behaviours, knowledge, skills and willingness to develop set the standard for your team.
Your professional development is a core component of managing a team and ensuring the delivery of safe, compassionate and high-quality care.
- Enhanced communication skills – Strengthens trust, clarity and team cohesion; improves patient and staff experience.
- Coaching Skills – Builds staff confidence and accountability by encouraging clearer thinking, reflection and practical problem-solving.
- Appraisal – Supports development, strengthens engagement and aligns goals with job descriptions.
- Recruitment – Ensures the right people join the team, improving culture, safety and retention.
- Mandatory Training (ESR) – Maintains workforce competency and compliance.
- DatixCymru – DIF 2 Training – Enables meaningful incident learning, trend analysis and safety improvements.
- Audit Systems – Assures quality, monitors standards and guides quality improvement.
- Finance Training – Strengthens resource management and supports safe, sustainable service delivery.
- Establishment – Ensures safe staffing, effective workforce planning and service resilience.
- Oracle – Supports transparent, efficient procurement and financial governance.
- Rostering – Improves staffing efficiency, wellbeing and continuity of care.
- HR Processes [Capability, Conduct, Respect & Resolution, Sexual Safety, Managing Attendance at Work (MAAW), Wellbeing] – Strengthen fair, consistent people management, ensuring staff are supported, concerns are addressed appropriately and a safe, professional and well-functioning team environment is maintained.
- Equality, Diversity & Inclusion – Understand EDI, legislation and its place in ensuring clinical areas are fair, free of unconscious bias and create inclusivity and diversity.
- Responding to Concerns – Ensures concerns are handled openly and appropriately.
- Compassionate Leadership – Strengthens psychological safety, engagement and team performance. Gives managers the skills to manage challenging and difficult conversations compassionately.
- Leadership Training – Enhances ability to influence culture, motivate others and lead change in the clinical areas. Professional development for nurses and midwives – HEIW.
- Management Training – Develops systems thinking, operational capability and service efficiency.
- Quality Improvement – Understand the processes to implement measurable, sustainable improvements in care quality and safety.


Leading on learning and development on your ward
As a Band 7 Ward Manager, you play a pivotal role in collaborating with education teams to ensure continuous professional development across your workforce, strengthening educational governance and capability so that your service can deliver safe, high-quality care in alignment with organisational and national priorities.
- Provide leadership to ensure that learning and development activity within the ward aligns with patient need, organisational strategies, regulatory requirements and national competency frameworks.
- Establish strong collaborative relationships with key stakeholders including the practice development teams, corporate education teams and practice education facilitators to support high-quality learning experiences, workforce development and continuous quality improvement in education.
- Ensure effective communication structures so that staff and learners have timely access to educational guidance, support and escalation pathways. Maintain clear visibility of key contacts and ensure these are embedded in local induction and onboarding materials.
- Support and encourage in-house education by working proactively with education teams to bring targeted developmental sessions to the ward that address themes from audit, incident trends, competency gaps or service transformation.
- Monitor compliance with mandatory training, clinical competencies and practice assurance requirements, escalating risks and taking action to address gaps.
- Support the development of link roles including student link nurses and practice education champions, ensuring they are appropriately trained, supported and integrated into education planning.
- Promote a culture of learning and innovation where evidence-based practice, reflective learning and professional growth are embedded within everyday activity.
Leading on pre-registration education
Student nurses are essential to the future workforce and 50% of their learning experience occurs in the clinical environments. Their experiences directly influence recruitment, retention and quality of care.
As a Band 7 Ward Manager, you hold accountability for creating a high-quality clinical learning environment that is safe, supportive, structured and aligned with NMC regulatory standards (NMC). Your leadership sets the tone for the ward’s educational culture.
- Ensure the ward consistently meets NMC standards for supervision and assessment and that educational quality is routinely monitored, evaluated and improved.
- Confirm students receive an induction and orientation to the clinical area, ensuring students receive a comprehensive introduction to the area, its routines, expectations, escalation processes and safety protocols.
- Ensure robust supervision arrangements, including allocation of trained Practice Supervisors and Practice Assessors in advance of placement start, with clear communication of roles, responsibilities and expected learning outcomes.
- Ensure Practice Supervisors and Practice Assessors are supported to accurately assess and sign off proficiencies to ensure learners are competent, safe, and ready for professional practice.
- Make information resources accessible to the students, such as a student information board or digital booklet outlining key contacts, learning opportunities, placement expectations and support processes.
- Safeguard students’ supernumerary status as mandated by the NMC.
- Facilitate a psychologically safe and inclusive learning culture, promoting curiosity, reflective practice and professional behaviours while ensuring students feel valued, respected and part of the team.
- Monitor the quality of the learning environment, gathering feedback from students, supervisors and assessors, taking timely action to address concerns, improve experience and address risks to learning.
- Act as a role model for professional excellence, demonstrating evidence-based practice, compassionate leadership and a commitment to lifelong learning that inspires future registrants.
Creating a learning culture
Why a learning culture matters
A learning culture is essential for safe, effective and compassionate care. As a Band 7 Manager, you are the cultural influence of the clinical environment. Your leadership directly influences how staff experience learning, how they respond to change, challenge and how they professionally develop. A learning culture is a way of working, thinking and leading embedded into everyday practice.
What a strong learning culture looks like
A learning culture should result in:
- Staff feel confident, valued and empowered.
- Mistakes lead to improvement, not fear.
- Learning becomes routine, not an event.
- Patient safety and continuous quality improvement to care delivery.
- Begin conversations with curiosity, not judgement: “Help me understand whathappened…”
- Thank staff for raising concern, even when the information is uncomfortable.
- Maintain confidentiality and fairness in all investigations.
- Ensure that everyone feels psychologically safe to ask questions and learn.
- Create an environment that values diversity, inclusivity and a collective approach to education
- Begin conversations with curiosity, not judgement: “Help me understand whathappened…”
- Display learning themes, improvements and successes on ward boards.
- Share “what we learned this week” updates.
- Celebrate improvements publicly.
- Link learning directly to clinical environment, patient outcomes and staff observations. Tailor educational sessions and conversations to real themes from Datix, audits and patient feedback.
- Use Datix reviews as reflective teaching, focusing on systems thinking rather thanblame.
- Introduce brief learning pauses at the end of a shift using coaching style questions: What went well? What challenged us? What do we take forward tomorrow?
- Empower deputies and senior staff nurses to lead learning conversations to buildresiliency and trust
- When patterns arise such as repeated falls or medication errors, encourage a collective and inclusive approach to define small, testable improvements using quality improvement principles.
- Provide time, support and visibility for staff-led change.
- Move from identifying issues to developing practical solutions.
- Ensure the team understand the changes arising from their contributions.
- Notice when staff need support, feedback, recognition and provide support
- Create opportunities for skill development, simulation and bedside teaching.
- Ensure learning opportunities are equitable, prioritising staff who may be overlooked or less confident.
- Incorporate short, focused discussions into safety briefings, handovers, posters and debriefs. Use every day as opportunities for learning and development.
- Encourage all team members to contribute to the learning culture healthcare supportworkers, students, newly registered nurses and senior staff all hold valuableperspectives and thoughts. An understanding of each role is essential to identify howall members of the clinical area will work cohesively to create a learning culture.
Enabling Continuing Professional Development
What is CPD?
Continuing Professional Development (CPD) is a lifelong, structured and reflective process of learning that enables the workforce to maintain, enhance and develop the knowledge, skills, competence, values and behaviours required for safe, effective and compassionate practice.
It includes a broad range of learning opportunities that may be self-directed, planned or unplanned, formal or informal, all of which contribute to professional growth through reflection and learning from real experiences in healthcare settings.
CPD supports individuals, in partnership with their organisation, to sustain existing practice, develop new capabilities and adapt to changing service needs. It also provides opportunities to gain recognition for learning and professional development, ensuring that knowledge and skills continue to evolve across the lifetime of a healthcare career while strengthening the quality and safety of care delivered.
What makes CPD so important?
- Safeguards the quality and safety of care for patients, service users and the public
- Ensures the workforce remains competent and responsive to evolving evidence-based practice, service models, population needs and national priorities in a complex healthcare environment
- Is critical to workforce sustainability, service transformation and the delivery of high-quality care
What are the requirements of CPD?
CPD is a shared responsibility between individuals and organisations. Individuals are expected to engage actively in their own learning, reflect on practice, identify development needs and apply learning to improve care. Organisations are responsible for creating the conditions that enable CPD, including equitable access to learning opportunities, appropriate support, recognition of learning and protected time where possible.
CPD should be aligned to service priorities, professional standards, regulatory requirements and organisational objectives, while remaining flexible enough to meet individual and team needs.
Key principles of CPD
The HEIW strategy (HEIW, 2023) outlines CPD as:
- Inclusive of all healthcare staff, roles and professions
- Embedded in everyday practice and work-based learning
- Valuing experiential, reflective and informal learning alongside formal education
- Aligned to quality improvement, service need and population health priorities
- Supported by shared responsibility between individuals and employers
- Recognised, recorded and evaluated to demonstrate impact on practice and outcomes
- Culture of CPD
70 – 20 – 10 Model
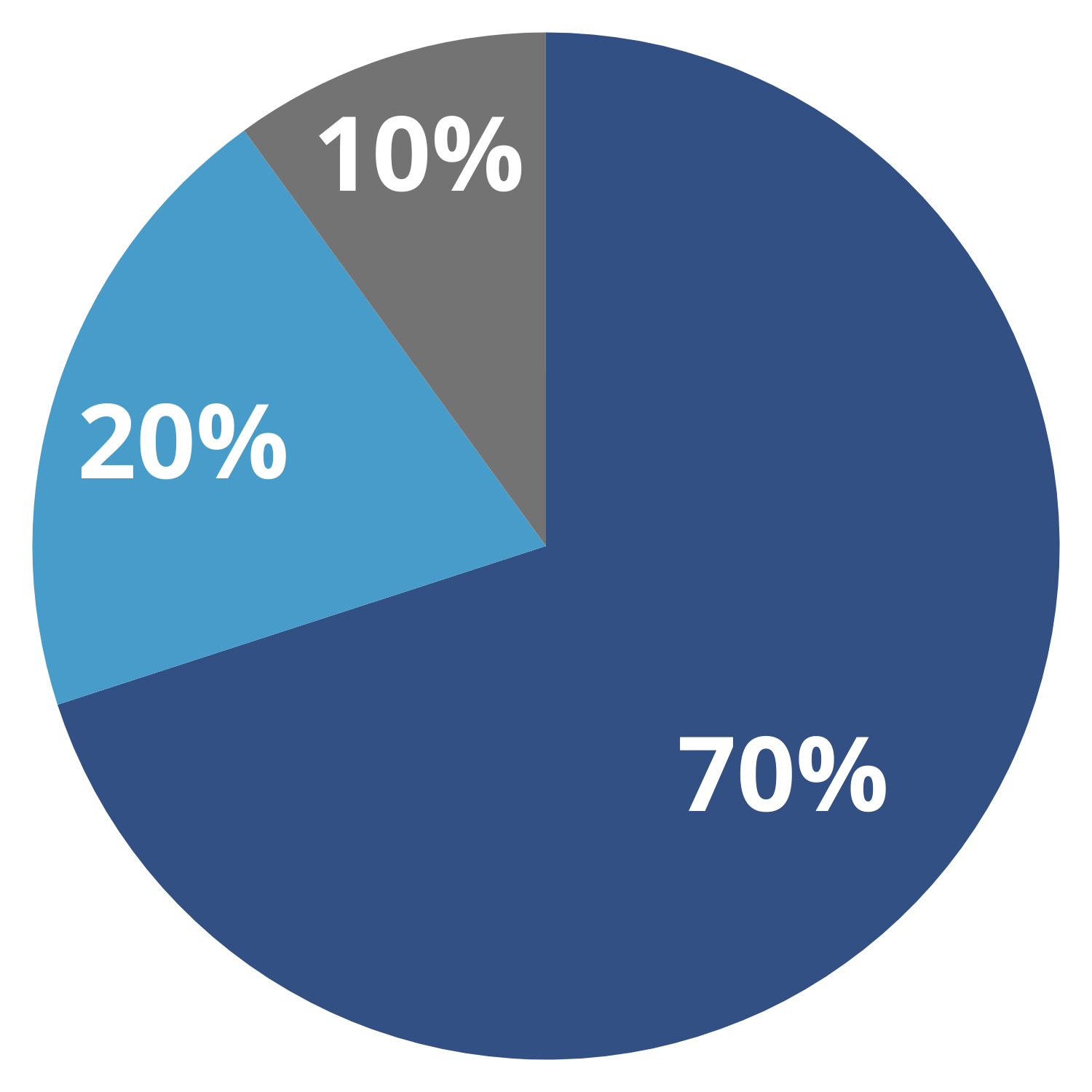
Managers should be aware of the 70–20–10 model, which reinforces that most learning does not come from formal courses but from an everyday learning culture (Mundt MH, Clark, & Klemczak, 2013).
It highlights that approximately 70% of development occurs through on-the-job experience, 20% through learning from others such as mentoring and only 10% through structured education (Bournes & Ferguson-Paré, 2007).
Understanding this model helps challenge the perception that formal training is the main source of learning and encourages managers to create rich, supportive learning opportunities within daily clinical work.
Understanding this model helps challenge the perception that formal training is the main source of learning and encourages managers to create rich, supportive learning opportunities within daily clinical work.
| On-the-Job Learning | Social Learning | Structured Education |
|---|---|---|
| 70%: Learning through experience | 20%: Learning through Others | 10%: Formal Learning |
|
|
|
Putting CPD into practice
Preceptorship
Preceptorship is a structured period of support that helps newly registered nurses andothers new to the UK, organisation, or specialty transition into safe, confident,autonomous practice. It provides guided learning, supervision, and feedback to help staffconsolidate skills and meet professional standards. Each Health Board/Trust providepreceptorship.
- Ensure preceptorship is in place: Allocate every newly registered or new‑to‑areanurse a trained preceptor and ensure they receive a structured induction andprotected supernumerary time as required.
- Create conditions for effective learning: Ensure preceptors have the time,resources, and support to deliver high‑quality preceptorship throughout theprogramme.
- Monitor progress: Review competency development, provide oversight of preceptor–preceptee activities, and step in early if additional support is needed.
- Promote confidence and integration: Maintain a supportive culture where new staffcan ask questions, reflect on challenges, and gradually build autonomy.
- Ensure consistency and quality: Align ward‑level preceptorship with nationalstandards and organisational policies, contributing to retention, safe practice, andconfident professional transition.
Restorative Clinical Supervision
Restorative clinical supervision is a reflective, supportive process that helps nursesexplore their emotional experiences at work, build resilience, and restore their capacity tothink clearly through guided reflection, supportive challenge, and action planning.
- Enable access and protected time: Ensure nurses can attend restorative supervision sessions without interruption and promote it as a routine part of wellbeing and reflective practice.
- Promote awareness: Make sure staff know who provides RCS (e.g., PNAs) and how to access sessions, using clear communication and signposting.
- Support supervisors/PNAs: Allow facilitators time within workload to deliver effective RCS and recognise their role in staff wellbeing.
- Foster a reflective culture: Encourage staff to use RCS to process challenges, reduce stress, and enhance compassionate care.

Website
Training Needs Analysis (TNA)
Collectively with your senior leaders and your education team, an annual training needsanalysis needs to be completed.
This assessment identifies the education and development required for current staffto maintain competence and meet evolving service needs. You need to consider whatis required and by what method.
Any education that requires funding or commissioning needs forecasting and forecastingthrough a TNA. You also play a crucial role in assessing future workforce demand so theycan anticipate the number and skill mix of staff needed moving forward, which informstraining places in the universities.
Digital Fluency
Many Nurses do not see themselves as digital and data literate despite using technologyand interpreting a variety of data daily, from vital signs to using electronic devises,entering information on clinical workstations or just helping patients call relatives onsmart devices.
Across nursing practice digital and technological innovation drives transformationalchange. These advancements are not merely operational upgrades; they are strategicenablers of safer, more efficient, and more person-centred care. From implementing theWelsh Nursing Care Record (WNCR) to ePrescribing, analytics, and hybrid workingmodels, digital tools are reshaping the landscape of healthcare delivery.
For you as ward managers, digital transformation presents both an opportunity and a leadership imperative. They are uniquely positioned to lead their teams through thisshift by modelling digital confidence, supporting staff development, and embedding newtechnologies into everyday ward practice.
- Welsh Nursing Care Record (WNCR): Enables bedside documentation via mobile devices, replacing paper-based forms and allowing for real-time, patient-centred assessments. Access training.

- Electronic Prescribing and Medicines Administration (ePMA): Electronic prescribing and medication administration reduce the risk of medication errors, enhance communication across teams, and support safer prescribing practices.
- NHS Wales App: Empowers patients to manage appointments, access test results, and engage with services more autonomously.
- Data and Analytics: Real-time dashboards and clinical data analytics support informed decision-making, performance monitoring, and service improvement.
- Flexible and Hybrid Working Models: Digital platforms are enabling new models of working, including remote access to records and virtual consultations, enhancing flexibility for staff.
- Welsh Language Compliance: Digital platforms are being designed in line with the Welsh Language Act (1993) to ensure equitable access to bilingual services.
- Reduces Administrative Burden: Automates routine tasks and documentation, releasing time to care and reducing cognitive load.
- Improves Accuracy and Efficiency: Reduces duplication, enhances legibility, and ensures contemporaneous documentation.
- Enhances Patient Safety: Real-time access to accurate information supports safe clinical decisions and reduces errors, particularly in medication management.
- Strengthens Professional Autonomy: Data-driven practice supports nurses in evidencing outcomes, contributing to service development, and engaging in reflective practice.
- Promotes a Positive Patient Experience: Digital tools streamline processes, reduce delays, and empower patients to participate actively in their care journey.
- Lead with confidence when using digital tools
- Encourage peer learning and build a team of digital champions.
- Spot learning gaps early and link staff to training.
- Encourage peer learning and build a team of digital champions.
- Include digital skills in appraisals.
- Co‑produce new digital ways of working with your team.
- Tackle anxieties with clear, consistent communication.
- Keep the “why” front and centre—better care, better working lives.
- Make sure no staff or patients are left behind due to digital exclusion.
- Use accessible formats and support those with low digital confidence.
- Use dashboards to track staffing, KPIs, discharges, and incidents.
- Integrate digital tools into board rounds, MDTs, and QI work

Website

Publication Long Read

Website
Webpage last updated on: 23rd May 2026



